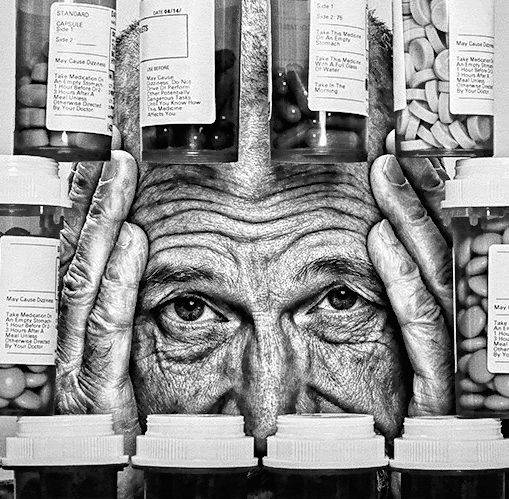
A Bladen County health provider acknowledges the medical profession is part of the opioid problem.
As part of the ongoing series on the opioid epidemic, the Bladen Journal reached out to people in a variety of fields — mental health, criminal justice, education, law enforcement, etc. — most of whom readily agreed to provide what insight they could offer into the current epidemic.
No field was more guarded, however, than the medical one, and only two of the six health providers contacted agreed to speak on the record. Three health providers either flatly refused to talk or didn’t return attempts to contact them.
An additional provider, referred to ficticiously here as Ben Singletary, agreed to speak under anonymity.
“I’m just tired,” he said. “I’m tired of being part of the problem.”
Singletary voiced concern on one hand that finger-pointing wouldn’t do any good in coming up with workable solutions — but on the other hand, he also stated that in order to fix any issue, the problem needs to be identified. And he sees the problem — at least part of it, anyway.
“I question whether I should (provide) prescriptions often,” he said. “Everybody does.”
When questioned how, then, addicts are able to get their hands on pills, he leaned back in his chair, then forward. He put his head on his knees, then raised up and covered his face with his hands. A long sigh. A full minute passed while he alternated nervously wringing his hands, running them across his face, and burying his face in his hands.
“I have to do the right thing,” he said with a mixture of determination and sadness. “This is the right thing to do.”
“We’re making money off of it,” he said at last, with the sigh of someone releasing a burden.
“I don’t know what will happen to me (financially). This is my livelihood, you know? And it’s hard enough making ends meet now. What will happen?” he questioned, with shoulders slumped.
Singletary called the opioid epidemic “frightening,” but acknowledged a large portion of his income comes from people returning for pills.
That the health industry is profiting from the opioid epidemic is nothing new. Such statements were levied by both the residents and the leaders at Carolina Crossroads — a drug rehabilitation center in Bladen County — as well as by the family of Brandon Owen, who was addicted to opioids and overdosed in February of this year.
“I’ve been saying that for a long time — that the health industry doesn’t want this problem to go away,” Doyle Owen commented. “I can’t believe one of them is actually admitting it though. I hope this will open people’s eyes.”
Far from just saying some health providers perpetuate the problem, however, Singletary said the problem now killing nearly 30,000 people every year in the U.S. stemmed from the very industry supposedly dedicated to saving lives.
“It’s been said at professional conferences that the fifth vital sign came about because pharmaceutical companies paid off legislators,” Singletary explained, referring to the addition of the question, ‘How would you rate your pain?’ to patient intake. “Once pain became a fith vital sign, the practice of prescribing opioids took off.”
The link between profit and the preponderance of the problem hasn’t been lost even on substance abusers. Gavin Kersey is a resident at Carolina Crossroads, where he checked into because of his opioid addiction.
“Pharmaceutical companies are the ones benefiting from opioid addiction,” he said pointedly.
At a recent planning session for Bladen County’s leadership forum on opioid abuse, one participant suggested another impetus to the crisis.
“Back in the 1980s, funding was driven by patient satisfaction scores,” said a local nurse. “If a person came into a hospital and said they were in pain, if you didn’t treat it, they would give you a bad patient satisfaction score, and funding was based on that score.”
Though the link between funding and patient satisfaction has been erradicated because of the endemic problems, the beast had been born — a society convinced pain is bad.
“Pain is a good thing,” said David Howard, Bladen County health director. “It’s your body’s way of telling you to take it easy and letting you know when you need to rest.”
If Singletary is right, however, the push behind pain medication — big pharma — and its message “You deserve to be pain-free” was too strong to withstand any attempt to convince consumers pain is a necessary and beneficial part of healing.
“If we didn’t have a lot of these opioids from the pharmaceutical industry, I don’t think the problem would be as bad as it is,” Singletary remarked. “And if I said that on the record, I would (be out of my profession), because they would come after me.”
Regardless of the reason, the effect was tremendous. According to the Department of Health and Human Services, in 1991, health professionals wrote 76 million opioid prescriptions in the U.S. By 2011, the number had increased to 219 million, while heroin production increased 500 percent from 2005 to 2009. Each day, 3,900 people initiate nonmedical use of opioids, and 580 use heroin for the first time. The U.S. — which comprises 5 percent of the world’s population — consumes 80 percent of the world’s opioids.
While the problem exists nationwide, North Carolina is doing its share. A 2016 study by Castlight Health, a San Francisco-based health care information company, rated the worst 25 cities nationwide for opioid abuse. No. 1 on the list was Wilmington, and Fayetteville made the list as well, at No. 18. Two other cities in North Carolina rounded out the problem areas, which, if reflective of larger data, means the Tar Heel State alone contributes approximately one-sixth to the nation’s opioid problem.
“It used to be that everyone coming in treatment centers was addicted to cocaine,” said David Chestnutt, director of Carolina Crossroads. “Now it’s opioids. I bet 80 percent of the guys here are addicted to opioids.”
For at least one health provider, enough is enough. Singletary, once his confession was out, was resolved that people know. Even when given the opportunity to rethink or double-check his statement, the health provider declined.
“If I do that, it won’t be honest,” he said. “What I’ve told you is the truth, and I don’t want the opportunity to go back and say it isn’t. I’m just tired, and I don’t want to do this any more.
“If we’re going to get serious about this, we have to start by being honest,” he added, “because denying what’s going on isn’t helping anyone.”
Chrysta Carroll can be reached by calling 910-862-4163 or emailing [email protected].